]]>
Development of autoimmunity at an early age associated with more aggressive form of the disease in genetically susceptible children, a USF Health-led study suggests
TAMPA, Fla. (Oct. 21, 2021) — New findings from the international The Environmental Determinants of Diabetes in the Young (TEDDY) study add to the growing body of evidence indicating that type 1 diabetes is not a single disease. The presentation and, perhaps, cause of autoimmune diabetes differs among genetically high-risk children, the research suggests.
In a cohort study published July 22 in Diabetologia, lead author Jeffrey Krischer, PhD, director of the Health Informatics Institute at the USF Health Morsani College of Medicine, and TEDDY colleagues compared the characteristics of type 1 diabetes diagnosed in children before vs. after age 6. The paper’s senior author was Beena Akolkar, PhD, of the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK).
“Our results underscore the importance of taking into account the age at development of multiple autoantibodies when evaluating risk factors for progression to a diabetes diagnosis,†said lead author Dr. Krischer, a Distinguished University Health Professor and co-chair for the National Institutes of Health-funded TEDDY consortium. “When the changing picture of autoantibody presentation is considered, it appears type 1 diabetes at an early age is a more aggressive form of the disease.â€
In type 1 diabetes, a misdirected immune response attacks and destroys insulin-producing beta cells in the healthy person’s pancreas – a process occurring over months or many years. Four autoantibodies directed against the pancreatic β-cells — glutamic acid decarboxylase autoantibody (GADA), insulin autoantibody (IA), insulinoma-associated-protein-2 autoantibody (IA2-2A), and zinc transporter 8 autoantibody (ZnT8A) – are thus far the most reliable biological indicators of early type 1 diabetes, before symptoms appear. Not all children who test positive for one or more autoantibodies progress to a diagnosis of type 1 diabetes, which requires lifelong administration of insulin to control blood sugar levels and reduce health complications.
Over the last decade, TEDDY researchers have learned more about how the order, timing and type of autoantibodies can help predict which genetically susceptible children are most likely to get type 1 diabetes as they age.
For this multisite study in the U.S. and Europe, the researchers analyzed data from 8,502 children, all at genetically high risk for developing autoimmunity and type 1 diabetes. The children were followed from birth to a median of 9 years. Over this period, 328 study participants (3.9%) progressed from a presymptomatic stage in which autoantibodies first appeared in their circulating blood (signaling initial autoimmunity) to the onset of symptomatic type 1 diabetes.

Study lead author Jeffrey Krischer, PhD, directs the USF Health Informatics Institute and is co-chair for the National Institutes of Health-funded TEDDY consortium.
Half of the 328 participants (2.0%) were diagnosed before age 6, while the other half (1.9%) developed diabetes between ages 6 and 12. The aim was to determine whether the younger group diagnosed with type 1 diabetes differed from the older group, which would suggest that a different form of type 1 diabetes emerges in children as they grow older.
Among the findings:
- As expected, TEDDY participants who progressed to diabetes between ages 6 and 12 were more likely to have first-appearing autoantibodies to the pancreatic enzyme glutamic acid decarboxylase (GAD autoantibodies), while first-appearing insulin autoantibodies (IA antibodies) were much more common in younger children developing the disease.
- The rate of progression to type 1 diabetes was slower if multiple (two or more) autoantibodies appeared after age 6 than if they were present before age 6.
- The significant association of country of origin with diabetes risk found in the younger group declined in the older group. Conversely, the link between certain genotypes and a higher likelihood of developing diabetes significantly increased in the older children.
- Among children 6 and older with multiple autoantibodies, family history did not appear to play a role in whether the child progressed to type 1 diabetes.
“Much of the observed differences in the relationship between genes and environmental exposures can be explained by the age at appearance of autoantibodies,†Dr. Krischer said. “That is important, because it means factors linked with diabetes risk need to be conditioned on age to be properly understood. There may be different environmental exposures occurring at different ages that trigger autoimmunity, or the same environmental trigger may act differently at different ages.â€
The research was funded by grants from the NIDDK and several other NIH institutes, JDRF, and the Centers for Disease Control and Prevention (CDC); and supported in part by NIH/NCATS Clinical and Translational Science Awards.
Â
]]>
]]>
The Environmental Determinants of Diabetes in the Young study is led by USF Health’s Jeffrey Krischer, who has built a worldwide epidemiological hub for T1D research at USF
TAMPA, Fla (July 11, 2021) — The National Institutes of Health (NIH) has awarded the University of South Florida total expected funds of $69.9 million over the next four years to continue the follow-up of study participants in The Environmental Determinants of Diabetes in The Young (TEDDY) consortium. TEDDY is the largest multicenter prospective study of young children with genetic susceptibility to type 1 diabetes (T1D).
The new grant from the NIH’s National Institute of Diabetes and Digestive and Kidney Diseases will also support a second case control study, building upon earlier TEDDY analyses examining how genetic factors and environmental exposures such as infectious agents, diet, and psychosocial stress affect T1D development in high-risk children. The extended project will incorporate viral biomarkers to help explain how viruses may trigger or contribute to the disease process.
Distinguished University Health Professor Jeffrey Krischer, PhD, director of the Health Informatics Institute at the USF Health Morsani College of Medicine, is the principal investigator for TEDDY. He has overseen the NIH-supported data coordinating center for this consortium since its inception in 2004. The Health Informatics Institute employs advanced technologies such as proteomics, epigenetics, gene expression analyses, and metabolomics for TEDDY and other NIH initiatives. Under Dr. Krischer’s leadership, USF has built an internationally recognized hub for epidemiological research in T1D.
A 2019 Nature Medicine paper by Kendra Vehik, PhD, and colleagues at the USF Health Informatics Institute, reporting on unexpected connections between viruses and autoimmune-related diabetes, was recently highlighted by Nature as one of 24 milestones in diabetes research over the last 100 years (milestone No. 23).
Type 1 diabetes is an autoimmune disease in which the body’s immune system attacks the pancreatic β-cells making insulin – a process that occurs over months or many years. The presence of autoantibodies (immune proteins) in circulating blood indicates that the body has begun targeting its own tissues or organs.
TEDDY researchers at six clinical centers in the U.S. and Europe have been following 8,500 children from birth up to age 15, with the aim of identifying environmental factors that influence autoimmune destruction of β-cells. Beta cell autoimmunity ultimately leads to the onset of T1D, which requires life-long insulin injections to treat symptoms.

A 2019 published discovery stemming from TEDDY research showed unexpected connections between viruses, like the enteroviruses illustrated here, and autoimmune-related diabetes. The paper by USF Health’s Kendra Vehik and colleagues was recently highlighted as one of 24 Nature Milestones in Diabetes. | Credit: Kateryn Kon
“Our TEDDY study group has made great strides in understanding the different biological pathways by which a child may develop diabetes-related autoimmunity,†Dr. Krischer said. “We are grateful to the many patients and families who collaborate in our studies. Their resolve inspires us to accelerate our efforts to pinpoint the mechanisms of type 1 diabetes, with the goal of preventing, delaying or reversing this life-altering condition.â€
The exact causes of TD1 are unknown. But TEDDY has more clearly defined combined risk factors that can help predict β-cell autoimmunity and T1D onset, including the rates of disease progression, and the distinct stages of type 1 diabetes development.
“Dr. Krischer and his team have provided valuable insights into the interplay between genetic and environmental factors underlying the complex disease process of autoimmune diabetes,†said Charles J. Lockwood, MD, senior vice president of USF Health and dean of the Morsani College of Medicine. “Their work, powered by a research platform supporting high-performance computing and big data, is rigorous and critically important for finding new treatments and preventive approaches.â€
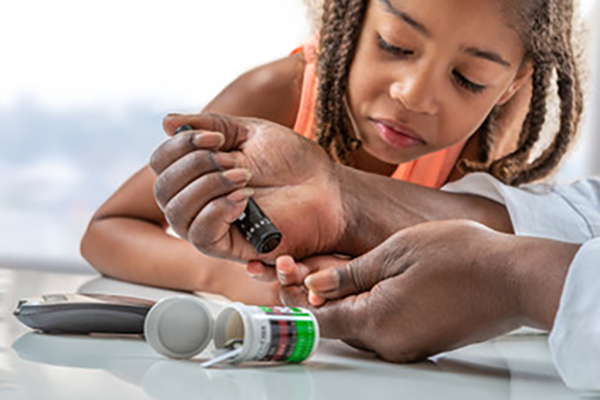
Children and adults with type 1 diabetes must monitor their dietary intake and exercise and take insulin injections, or use an insulin pump, daily to help control their blood sugar levels.
Key discoveries from TEDDY investigations over the last several years include:
- Maternal stress during pregnancy and child’s T1D genetic risk: Certain psychological stress during pregnancy (interpersonal and job-related life events) are differentially related to first-appearing autoantibodies –insulin autoantibodies (IAA) vs. glutamic acid decarboxylase autoantibodies (GADA). Excess T1D risk often depends upon specific interactions between the mother’s environmental stress and the child’s genes.
- Distinct autoantibody spreading and progression to disease: Detailed information about the order, timing and type of autoantibodies appearing after the first autoantibody can significantly improve prediction of which children are most likely to advance from initial autoimmunity to symptomatic T1D more rapidly.
- A possible infectious cause of diabetes: In young children at increased genetic risk for T1D, prolonged enterovirus infection plays a role in the development of autoimmunity that precedes T1D diagnosis.
- Human gut microbiome in early-onset T1D: For the first time, TEDDY extensively  characterized the developing gut microbiome (collection of bacteria, viruses and other microorganisms inhabiting the gastrointestinal tract) in relation to T1D. The work laid the foundation to identify gut microbes that may predict, protect against. or cause T1D risk or disease progression.
- Gene-environment interactions modify risk of diabetes-related autoimmunity: In TEDDY children up to age 6, T1D-related immunological changes were clearly dependent upon the interactions of genetic factors and environmental exposures that give rise to IAA or GADA as the first-appearing autoantibodies.
- Linking early supplemental probiotics with T1D autoimmunity: Early intake of probiotics, potentially helpful in maintaining the balance of gut microbes, may decrease the risk of autoimmunity in children at highest genetic risk for T1D. Further studies are needed before probiotic supplementation could be recommended.
***
The new grant is funded by the National Institute of Diabetes and Digestive and Kidney Diseases of the NIH under Award Number U01DK128847.
]]>


