Emergency L&D drill delivers dramatic dose of reality
The Department of Pediatrics new simulation center emphasizes multidisciplinary team training for routine and crisis medical scenarios
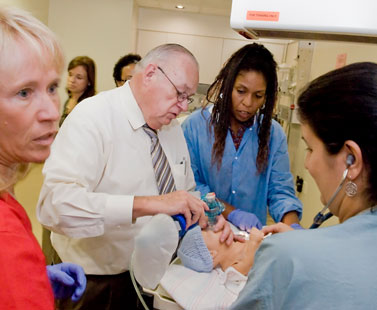
Dr. John Curran works with a team of residents and neontal nurse to stabilize a “newborn” during a recent emergency simulation exercise at the TEAMS Center.
It was a delivery room complication. The full-term newborn had inhaled meconium, its own feces, on its way out the birth canal and was having trouble breathing.
In a nearby room, USF Health Associate Vice President Dr. John Curran, a veteran pediatrician and neonatologist, was touring the Department of Pediatrics new Team Education and Multidisciplinary Simulation (TEAMS) Center with guest and colleague Dr. David Tayloe, president of the American Academy of Pediatrics. The 2,300-square-foot facility houses more than $250,000 worth of high-fidelity patient simulators – adults, a child and newborns – each with a computer-driven age-appropriate physiology that can mimic routine and crisis medical scenarios. The life-like mannequins can convulse, turn blue around the mouth, reproduce breathing sounds, recreate variations in blood pressure and heart rate, even secrete blood and other imitation bodily fluids.
With Dr. Tayloe at his side, Dr. Curran was unexpectedly whisked away to the simulation center’s labor and delivery room, where a team of USF neonatologists and an NICU nurse were already working on the tiny patient in distress – a newborn mannequin hooked up to a beeping monitor. In a nearby bed, the mother, an adult-size mannequin, shouts out: “What’s going on with my baby? Is he alright? Why won’t anyone tell me anything?”

Dr. Curran suctions and opens the airway.
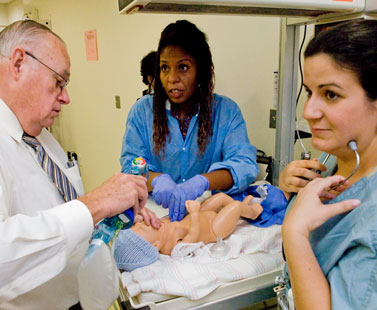
Dr. Curran begins ventilation as USF neonatology fellow Dr. Cathy Kotto-Kome performs chest compressions. Assisting at left is neontalogy fellow Yahdira Rodriguez-Prado.

Dr. Latha Kumaraswamy, a neonatology fellow, loads a syringe with epinephrine.
As the senior physician, Dr. Curran steps in to open the newborn’s airway by inserting a breathing tube. When the newborn’s heart rate continues to fall after the tube is inserted, ventilation and CPR compressions are begun. A succession of rapid-fire questions and commands cuts through the tension. Dr. Curran: “Where’s the oxygen?…Give me a good-size tube; you have all kinds of smaller ones.” Nurse: “Have we confirmed placement of the tube?” Neonatology fellow: “It’s good!” Dr. Curran: “Let’s get an umbilical cord line in.” Nurse: “Can we get a dose of epinephrine?” Neonatology fellow: “Epi in.” Nurse: “Heart rate coming up… Let’s call NICU and tell them we’re bringing a baby over and have a ventilator ready!”
Outside the room, TEAMS Center Director Laura Haubner, MD, and coordinator Jason Fields, punch up different angles of the scene on a computer monitor for better views of the team at work and control the infant’s vital signs as the drill unfolds. Once Dr. Haubner is satisfied with the team’s response, she brings up the baby’s heart rate with a few clicks of the computer mouse.

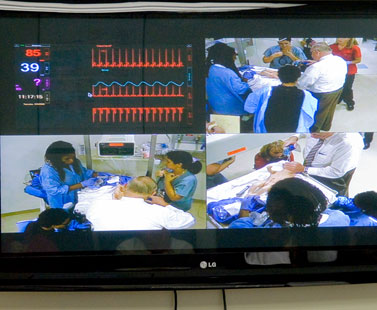
Above: USF pediatrician Dr. Laura Haubner, director of the TEAMS Center, and Jason Fields, center coordinator, monitor the team’s responses from a control station outside the L&D room. Below: They punch up different views on a computer screen as the emergency scenario unfolds and record for evaluation after the simulation exercise.
Following the emergency scenario, Dr. Haubner ushers the team and residents who observed the simulation into the center’s conference room, where she facilitates a debriefing. The health professionals watch a replay of their performance on a giant screen, critique their strengths and weaknesses, and discuss what they’ve learned. Dr. Haubner prods with questions: “When the heart rate dropped to 35, what were you thinking?… Were the chest compressions and ventilation well coordinated?… Do you feel you called for help readily enough?”
The debriefings are often an “eye-opening” experience for physicians and nurses, said Dr. Haubner, an assistant professor of pediatrics. “The teaching points elicited by the videotape can be very powerful. They get a sense of how important it is to set roles for each team member in advance and clearly designate a team leader.”

Dr. Haubner leads the team in a post-simulation debriefing, where members can critique their performance replayed on a giant screen.

Seated next to Dr. Terri Ashmeade (left), USF assistant professor of pediatrics and TGH NICU medical director, and Jason Fields (right), TEAMS coordinator, Dr. Curran poses a question to the group based on a rare, real-life delivery complication he experienced.
The center is intended to do more than allow physicians, nurses and medical students to practice, hone or retool their clinical skills in an environment without risk to real patients. “We strategically teach them how to deal with conflict and emotional distractions in both routine and crisis situations,” Dr. Haubner said.
The simulation team training focuses on multidisciplinary group dynamics, leadership, interpersonal communications skills and decision making under pressure, and emphasizes using all available information, equipment and people to achieve safe and efficient outcomes. “This crew resources management approach has traditionally been used by high stakes industries like aviation and nuclear power for simulation training, but it’s slowly being adapted by medicine, Dr. Haubner said. “We’re pretty high stakes too.”
The potential benefit for patient safety and improved outcomes is huge, she said. “According to the Institute of Medicine, most medical errors are based on lack of teamwork and miscommunication, not caused by inadequate medical knowledge.”
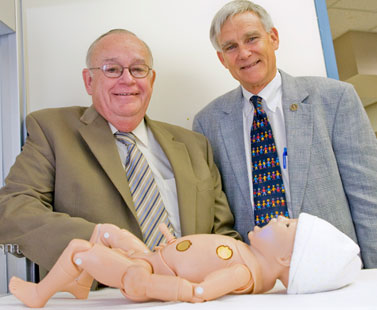
Dr. Curran with Dr. Paul Tayloe, president of the American Academy of Pediatrics, who observed the emergency L&D simulation during his visit to the TEAMS Center July 23. Dr. Tayloe earlier that morning had delivered the annual John S. Curran Lectureship, speaking to USF pediatrics faculty and residents about health reform.
Dr. Tayloe, who observed the emergency scenario and debriefing, was impressed by what he saw. “This is great. I can see how this type of simulation training would help take a lot of the anxiety out of having to walk into a real-life emergency and respond effectively as part of a team,” he said. “But keep in mind, if you find yourself practicing in a rural area, usually you are the team and must be able to save a baby’s life on your own. I still advise residents to take plenty of call in the delivery room!”
Housed on the first floor of the 17 Davis Building, the TEAMS Center formally opened July 1 and is operated by the Department of Pediatrics with support from the Office of Graduate Medical Education. It has been used by more than 130 USF faculty, residents and fellows — primarily from Pediatrics, Internal Medicine and Emergency Medicine — as well advanced registered nurse practitioners and respiratory therapists from Tampa General Hospital. The center expects to expand its simulation training to more health professionals and disciplines in the coming months, Dr. Haubner said.
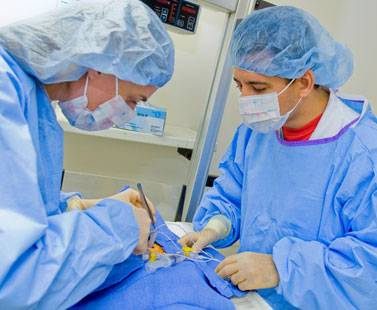
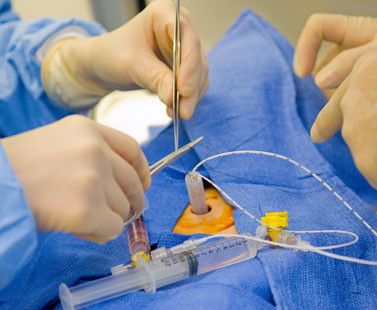
Using one of the center’s task-trainer simulators, third-year pediatrics resident Dr. Karolina Dembinski practices placing an umbilical catheter, used to deliver medications and fluids to critically ill infants, as neonatology fellow Luis Munoz observes.
In addition to Dr. Haubner and Jason Fields, TEAMS Center faculty include Brad Peckler, MD, from Emergency Medicine (Team Health), and Erika Abel, MD, USF assistant professor and program director of Med-Peds. For more information, please contact Dr. Haubner at lhaubner@health.usf.edu, or Jason Fields at jfields@health.usf.edu.
– Story by Anne DeLotto Baier, USF Health Communications
– Photos by Eric Younghans, USF Health Communications

