USF Health has established a Neurocardiogenetics Clinic focused on improving the quality of life for patients with hereditary neuromuscular disorders who are at risk for or already experiencing cardiac complications. Innovative genetic research is a central component of the new clinic.
The multidisciplinary clinic teams faculty and staff with clinical expertise in cardiology, genetics and neurology. The clinic is directed by Aarti Patel, MD, assistant professor of cardiology and director of the Cardiac Imaging Fellowship Program at USF Health in collaboration with Thomas McDonald, MD, professor of cardiology and molecular pharmacology and physiology, and a member of the USF Health Heart Institute, and Theresa Zesiewicz, MD, professor of neurology and director of the USF Health Ataxia Research Center. Patients receive a complete cardiac examination and testing along with a comprehensive family genetic evaluation from providers familiar with their neurological history.
“Combining all that information, we are able to come up with a personalized treatment plan,” Dr. Patel said.
Many patients initially seen at the Neurocardiogenetics Clinic have been diagnosed with Friedreich’s ataxia (FA), a rare, debilitating and life-shortening neuromuscular disorder that usually strikes in childhood. At some point in their lives 55 to 60-percent of FA patients develop some form of cardiac disease. The most devastating of these is cardiomyopathy, a heart muscle disease that limits blood pumped to the rest of the body and increases risk for heart failure and abnormal heart rhythms.
“FA is a multisystem disease that affects many different parts of the body, including the heart,” Dr. Zesiewicz said. “And one of its most sinister complications is cardiomyopathy, an enlarged heart.”
The Neurocardiogenetic clinic offers patients and their families the opportunity to participate in ongoing genetic studies exploring potential links between heart disease and neuromuscular diseases like FA and certain types of other ataxias and muscular dystrophies.

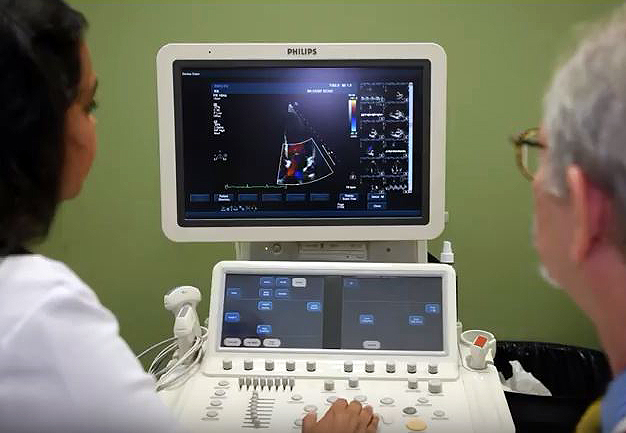
Dr. Aarti Patel (left), assistant professor of cardiology, collaborates with Dr. Thomas McDonald, professor of molecular pharmacology and physiology, at the new USF Health Neurocardiogenetics Clinic. Dr. Theresa Zesiewicz. professor of neurology (not pictured), is another collaborator.
While a deficiency in the frataxin protein can lead to fibrosis and scarring of heart muscle tissue in FA, competing theories exist about how a genetic mutation may actually result in heart problems in this particular ataxia and other neuromuscular disorders.
Dr. McDonald’s research team is searching for answers to many questions, including how different genetic variations may lead to cardiac abnormalities and affect the severity of heart disease.
Small blood samples are collected from patient volunteers with different inherited neuromuscular and/or cardiac disorders, as well as family members who are unaffected genetic carriers of neuromuscular diseases. In laboratory cell culture dishes, USF Health researchers genetically reprogram the blood cells into pluripotent stem cells that can grow into any cell type. Then they induce these stem cells — containing the same genetic make-up as the patient who provided blood — to become nerve cells and heart muscle cells.
The goal is to work out at a molecular level how FA or other inherited neuromuscular diseases damage the heart muscle. Once that is achieved, Dr. McDonald said, the “disease in a dish” can be used to identify potential drug targets and test treatment options on the patient’s own cells.
“With stem cell technology and disease-in-a-dish modeling, we’re looking for the earliest changes in either a heart or a nerve cell (that lead to disease),” he said. “A big unanswered question is whether the molecular or cellular process happening in the nerve is the same as that damaging the heart muscle. By using stem cell-based research we hope to be able to determine if there is a connection between the nerve and the heart – or whether it’s a separate, independent process but based upon the same genetic defect.”
The collaborative research builds upon robust data collected by doctors in the clinic, including the wide range of symptoms seen in patients with hereditary neurological disorders involving cardiac complications.
Ultimately, that can help improve understanding of why genetic variations in certain neuromuscular diseases cause cardiac complications, Dr. McDonald said. “Having a clear clinical picture of each research participant will help us correlate the genetics and function of cells we see in the laboratory with how that translates to disease progression in the individual.”
“With careful clinical surveillance and novel biomarkers, our hope is that we will be able to predict which patients and their family members are at highest risk for cardiovascular disease so we can intervene early with effective treatment,” Dr. Patel said. “We’re hoping to identify patients even before they develop cardiac symptoms, so we can prevent heart disease.”
-Video and photos by Allison Long, USF Health Communications and Marketing